Medically reviewed by
Dacelin St Martin, MD
Triple board-certified in Sleep Medicine,
Internal Medicine, and Pediatrics.
What is Wearable Technology? | Apple Watches can Save Lives | What is Sleep Apnea? | Effective Treatments
Overview
Waking up tired might be your new norm, one that you contend with by guzzling coffee and energy drinks.
Slowly but surely, you notice that this driving fatigue is wreaking havoc on your life. You’re nodding off while driving, having trouble remembering things, and your calm demeanor has been replaced by volatility. Friends and coworkers keep you at arm’s length to not unintentionally “poke the bear.”
Unfortunately, life has become a nightmarish escapade marred by exhaustion, with new symptoms lurking around the bend, ready to drain your remaining ounces of fortitude.
Morning migraines coupled with insatiable hunger have you at an all-time low. You feel exhausted. What could be causing this to happen? What could be making you so tired when you just got up from bed. Could sleep be the problem?
You read online that sleep can be monitored via your Apple Watch, and this is where things get interesting. You decide to take matters into your own hands and track your sleep to identify any problems. Luckily the Apple Watch sitting on your wrist has various tools to keep track of your sleep while you sleep.
What is Wearable Technology?
It’s safe to say that Apple Watches are on-trend, not just because they are aesthetically appealing, but because they allow you to monitor your health and sleep and detect underlying disorders.
A recent study suggests that wearables, such as the Apple Watch, Fitbit, and others, can monitor vital health signs like heart rate, pulse, blood pressure, respiratory rate, and continuous blood oxygen levels.
For example, you’re fine if your blood oxygen saturation is above 95 percent, but once you fall below this threshold, your body falls into distress, manifesting as shallow breathing, rapid heart rate, and high blood pressure.
What’s scary about low oxygen levels is that symptoms happen when you’re most vulnerable, curled up in bed, and fast asleep. Your body fights to transport oxygen to every living cell, and in severe cases, it can cause your brain and heart to malfunction, leading to heart attack, stroke, or sudden death.
But, you ask, how can an Apple Watch detect this physiological chaos? An Apple Watch can conveniently measure oxygen levels at your wrist via an oximeter while tracking other data, including respiration, via a built-in accelerometer. With an Apple Watch, you can track the number of breaths you take per minute while you sleep.
You can see your sleep health data plotted in the Health app; however, an app called Deep Heart takes technology even further by analyzing your data, comparing it to medical data from a large pool of people to detect abnormalities in your breathing and sleep.[6]
Apple Watches can Save Lives
Who knew that your Apple Watch could glean insight into unsatisfying sleep? Sure, it’s great for counting steps and calories, but you have to admit: sleep monitoring is the next level, a game-changer for your health.
After setting your sleep and wake times for the next two weeks, you crawl into bed. You wake up your first morning and check your sleep app, and the data jolts you awake.
Your blood oxygen levels are hovering around 82%; respiratory rate data shows that your breathing paused 60 times; and your blood pressure is through the roof at 180/110.
Your Apple Watch has detected that something is amiss with your health, and those hungry vibes you’ve been experiencing could be symptoms of an insidious sleep disorder that strikes at night and robs you of daytime acuity.
You have the raw data but no idea what it means, so you must speak with your doctor. A visit to SCOFA.com puts obstructive sleep apnea (OSA) on the radar, a potentially fatal sleep disorder that affects millions of Americans each year and often goes undiagnosed.
Your doctor suspects OSA after looking at your data and a brief physical exam, identifying your predisposing risk factors; however, what’s critical is having a proper diagnosis, whether from a home sleep test or an in-lab sleep study called a polysomnography.
What is Sleep Apnea?
A home sleep test confirms what your doctor suspected and supported the data shown on your app: OSA; however, the diagnosis has led to more questions, like what is OSA and how is it treated.
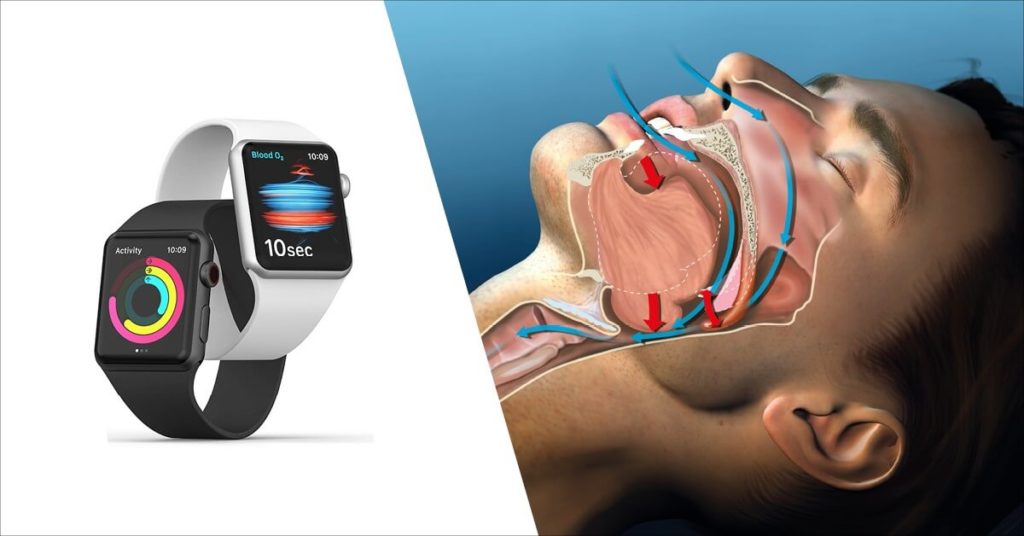
What happens is that the tissues in the back of your throat intermittently block your upper airway while you’re sleeping, causing your breathing to pause up to 300 times a night. Your body senses lower oxygen levels, sending signals to your muscles to wake up so you can get the air you need to breathe.
Because you’re asleep, you don’t realize that your breathing and sleep are disturbed; however, your symptoms speak volumes. You experience daytime fatigue because the nightly sleep disruptions prevent you from entering REM sleep, the most restorative sleep phase. Your killer morning headaches result from low blood oxygen levels and high blood pressure, which also strain your cardiovascular system.
You know when something is wrong with your body; however, having an everyday item readily on hand, like an Apple Watch, lets you track your sleep data and raises red flags when there’s an issue.
The health effects of this chronic sleep disorder are expansive and include diabetes, obesity, heart disease, stroke, and depression. Scarily enough, in severe cases, sleep apnea can even lead to spontaneous death.

Effective Treatments
Now, your Apple Watch has forever changed your health for the better. Sure, your journey to wellness started with symptoms, but this new technology gave you the data to back up your suspicions.
Various treatments are available, including the gold standard called continuous airway pressure (CPAP). Or you can opt for an oral appliance shaped like a mouth guard, which opens airways by advancing your jaw. Plus, there are surgery options, like upper airway stimulation.
Once you and your doctor decide on your treatment, your sleep will improve and your health. Until then, keep your Apple Watch handy. You don’t know when it can save your life.
Please keep in mind that although an Apple Watch is a great first-line tool for detecting sleep disorders, like sleep apnea, it’s not a replacement for physician care or medical diagnostics.
Click here to find a local sleep medicine doctor.
References:
[1] Gutierrez G. Cellular effects of hypoxemia and ischemia. In: The Lung: Scientific Foundations, 2nd ed, Crystal RG, West JB, Weibel ER, Barnes PJ (Eds), Lippincott-Raven Publishers, Philadelphia 1997. p.1969.
[2] Hornbein TF. Hypoxia and the brain. In: The Lung: Scientific Foundations, 2nd ed, Crystal RG, West JB, Weibel ER, Barnes PJ (Eds), Lippincott-Raven Publishers, Philadelphia 1997. p.1981
[3] Xie, J., Covassin, N., Fan, Z., Singh, P., Gao, W., Li, G., Kara, T., & Somers, V. K. (2020, April 13). Association between hypoxemia and mortality in patients with COVID-19. Mayo Clinic Proceedings. Retrieved May 19, 2022, from https://www.mayoclinicproceedings.org/article/S0025-6196(20)30367-0/fulltext
[4] Adeyinka A, Kondamudi NP. Cyanosis. [Updated 2021 Dec 13]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482247/
[5] Chatterjee, NA, Jensen, PN, Harris, AW, et al. Admission respiratory status predicts mortality in COVID-19. Influenza Other Respi Viruses. 2021; 15: 569– 579. https://doi.org/10.1111/irv.12869
[6] Ballinger, Brandon. “Screening for Hypertension and Sleep Apnea with DeepHeart.” Medium, Cardiogram, 2 Aug. 2018, https://blog.cardiogr.am/screening-for-hypertension-and-sleep-apnea-with-deepheart-416c9bc03efc.

