Medically reviewed by
Dacelin St Martin, MD
Triple board-certified in Sleep Medicine,
Internal Medicine, and Pediatrics.
Who Needs a Sleep Study | Disorders & Sleep Studies | Types of Sleep Studies |
Home Sleep Apnea Testing | Multiple Sleep Latency Test (MSLT) | CPAP Titration
Overview
If you’re having trouble sleeping at night or staying awake during the day, then you might need a sleep study to diagnose an underlying sleep disorder.
Sleep medicine specialists use different types of sleep studies to diagnose sleep disorders.
Polysomnography, Multiple Sleep Latency Test (MSLT), and home sleep tests help your sleep doctor diagnose potential sleep disorders.
Keep reading to learn more about the different types of sleep studies, how they’re done, who might need them, and what to expect during your test.
Who Needs A Sleep Study?
Signs and symptoms that you might need a sleep study include:
- Excessive daytime sleepiness
- Trouble concentrating during the day
- Loud snoring when asleep
- Trouble falling asleep
- Difficulty maintaining sleep
- Feeling irritable during the day
- Spontaneous sleep when reading or watching television
- Daytime fatigue
If you’re experiencing any one or more of these symptoms, then you might have a sleep disorder.
Your sleep doctor will recommend one or more sleep tests to evaluate the health of your sleep and diagnose any sleep conditions.
Disorders & Sleep Studies
Sleep studies can help diagnose a wide variety of sleep-related illnesses, such as:
- Obstructive sleep apnea (OSA)
- Central sleep apnea (CSA)
- Insomnia
- Hypersomnia
- Restless leg syndrome (RLS)
- Narcolepsy
- Sleep-wake cycle disorders
- Sleepwalking and talking
Depending on your symptoms, your sleep specialist will recommend one or more sleep tests to establish a diagnosis.
Types of Sleep Studies
Polysomnography
In-laboratory polysomnography also called monitored polysomnography, is the gold standard in sleep medicine.[1] It provides your sleep specialist with detailed physiologic measures to diagnose sleeping disorders.
If your sleep doctor suspects that you have sleep-wake cycle problems, sleep breathing disorders, sleep movement disorders, or any other type of sleep troubles, they will likely recommend monitored polysomnography.
How Is Polysomnography Performed?
During polysomnography, you will be scheduled to come to the sleep clinic at night around your usual bedtime. You will be given a private bedroom, where you can change into pajamas and get settled in for the night.
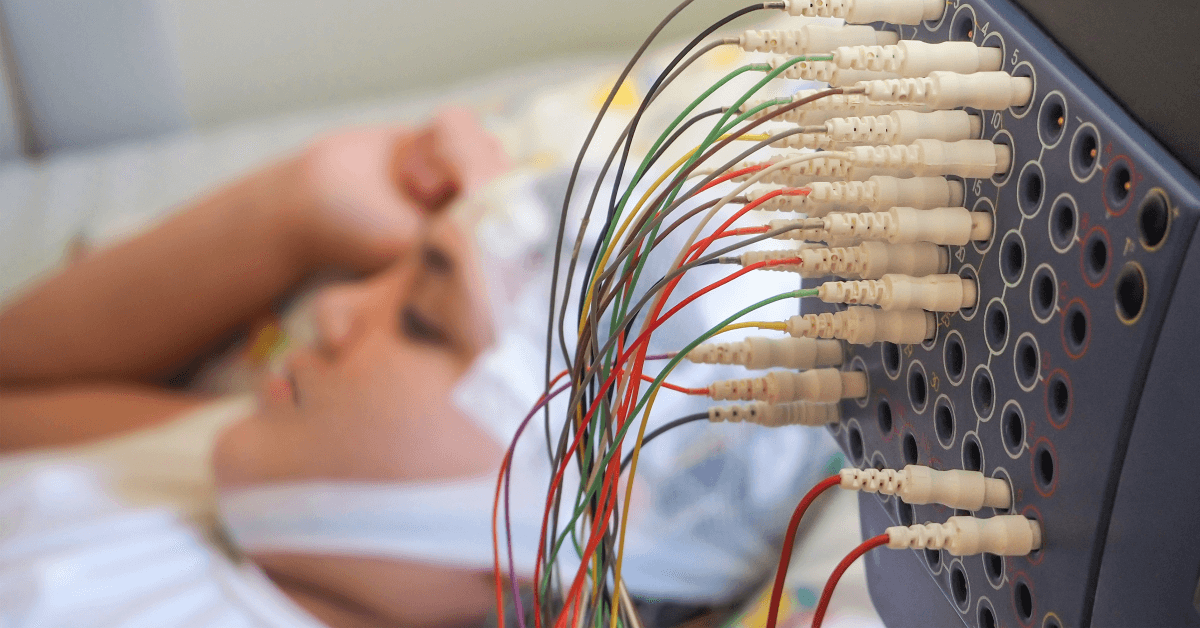
Before sleeping, the sleep technician will attach adhesive patches to your temples, chest, legs, and scalp. These patches contain sensors to measure different physiological variables as you sleep, which we will address later in this article.
The test usually takes the whole night, during which a sleep technologist will monitor you. You will be discharged in the morning once the test is complete.
In full-night polysomnography, the whole night is dedicated to measuring variables and establishing a diagnosis.
If you have obstructive sleep apnea (OSA), you will be asked to come for a second night to adjust your CPAP breathing device (CPAP titration). This protocol is the preferred treatment for sleep apnea and other sleep disorders.
A split-night polysomnography, however, is now being implemented as an alternative to a full-night sleep study.
The first part of your sleep (usually 3 hours) is dedicated to establishing a diagnosis. During the second part, the CPAP will be titrated. In this protocol, both the diagnosis and CPAP titration are done during the same night.
Split-night polysomnography is a viable option in some patients with severe obstructive sleep apnea.[2]
Polysomnography Measurements
During polysomnography, many physiologic measures are monitored and recorded:
- Electric brain activity
- Body movements
- Breathing rate and pauses
- Snoring and breathing sounds
- Eye movements
- Heart rate
- Blood oxygen levels
- Breathing pattern
Your sleep specialist will analyze the findings to establish a diagnosis. They will look for abnormal sleeping events, such as paused breathing, choking, awakening, and snoring.
Based on the variables, they will calculate scores, such as the Apnea-Hypopnea Index (AHI) in obstructive sleep apnea, to determine the severity of the diagnosed disorder.
Home Sleep Apnea Testing
Home sleep testing for sleep apnea is becoming popular in patients who fit specific criteria. It’s more cost-effective and allows patients to test themselves at home without sleeping in a sleep clinic.[3] A home sleep test device measures much fewer variables compared to in-laboratory polysomnography.
On the test night, you will attach the device to your body. Finger, nose, and chest sensors will measure your breathing efforts and blood oxygen levels.
Your sleep doctor will interpret the results. Based on the numbers, you will be scheduled for a CPAP titration to adjust your breathing machine.
Who Qualifies for Home Sleep Testing?
You might be eligible for home sleep apnea testing if:
- Your sleep doctor suspects that you have moderate or severe obstructive sleep apnea
- You don’t have symptoms of other non-respiratory sleep disorders, like narcolepsy or restless legs syndrome
- You are not a mission-critical worker, like an airplane pilot
- You don’t have additional medical conditions that might be contributing to your sleep-breathing disorder [4]
One company that provides home-sleep testing is MHSleepTesting.com. They will walk you through the process to ensure the diagnosis is fast and easy.
Multiple Sleep Latency Test (MSLT)
A multiple sleep latency test (MSLT) is prescribed for excessive daytime sleepiness patients.
Your sleep medicine specialist will order MSLT if they suspect you might have narcolepsy or hypersomnia, two disorders that make you fall asleep when you should be awake.
How Is A Multiple Sleep Latency Test Performed?
A multiple sleep latency test is a full-day test; it can take approximately 7 hours to perform. It’s done during the daytime when you usually should not be sleepy.
The test consists of 5 scheduled naps, approximately 2 hours between nap times. On each attempt to nap, you will be given 20 minutes to fall asleep.[5]
You will be woken up after 15 minutes of being asleep. Then you’ll wait for the following nap time to repeat the process.
During MSLT, you will be connected to sensors to measure your eye movements and brain activity. These sensors allow your sleep specialist to know how quickly you’re falling asleep and whether you’re reaching REM-stage sleep or not.
CPAP Titration
After full-night polysomnography or home sleep testing, your sleep specialist will need to adjust your CPAP device to match your needs. It’s done at a sleep clinic using the same polysomnography setup but with you wearing the CPAP mask.
As you sleep through the study, the CPAP pressure is adjusted to effectively prevent breathing pauses and airway collapse, effectively counteracting sleep apnea.
Summary
Sleep medicine involves several tests that help your sleep doctor establish a diagnosis and recommend suitable treatment.
Polysomnography is the most comprehensive of all sleep studies. However, you may be eligible for home sleep apnea testing as an alternate.
Either way, a CPAP titration study will usually follow to adjust your CPAP breathing machine to your needs.
If you have symptoms of excessive daytime sleepiness, then a multiple sleep latency test might be ordered. It’s done during the day and will help diagnose hypersomnia and narcolepsy.
In any case, if you suspect that you have any sleeping disorder, you should never delay consulting a sleep specialist. Unhealthy sleep can lead to chronic health conditions and affect your quality of life.
References:
- Kapur VK, Auckley DH, Chowdhuri S, et al. Clinical Practice Guideline for Diagnostic Testing for Adult Obstructive Sleep Apnea: An American Academy of Sleep Medicine Clinical Practice Guideline. J Clin Sleep Med JCSM Off Publ Am Acad Sleep Med. 2017;13(3):479-504. doi:10.5664/jcsm.6506
- Khawaja IS, Olson EJ, van der Walt C, et al. Diagnostic accuracy of split-night polysomnograms. J Clin Sleep Med JCSM Off Publ Am Acad Sleep Med. 2010;6(4):357-362.
- Chai-Coetzer CL, Antic NA, Hamilton GS, et al. Physician Decision Making and Clinical Outcomes With Laboratory Polysomnography or Limited-Channel Sleep Studies for Obstructive Sleep Apnea: A Randomized Trial. Ann Intern Med. 2017;166(5):332-340. doi:10.7326/M16-1301
- Rosen IM, Kirsch DB, Carden KA, et al. Clinical Use of a Home Sleep Apnea Test: An Updated American Academy of Sleep Medicine Position Statement. J Clin Sleep Med JCSM Off Publ Am Acad Sleep Med. 2018;14(12):2075-2077. doi:10.5664/jcsm.7540
- Carskadon MA, Dement WC, Mitler MM, Roth T, Westbrook PR, Keenan S. Guidelines for the multiple sleep latency test (MSLT): a standard measure of sleepiness. Sleep. 1986;9(4):519-524. doi:10.1093/sleep/9.4.519